The Placenta
A Selfless Servant
Most people give little thought to the placenta, and few appreciate the marvelous complexity and profound importance of this organ that is discarded and forgotten after birth.
In the Apostle Paul’s letter to the Romans, he compares the Church to the human body (Romans 12:4–8). The Church is one body made of many members, each having his own God-given gift. Likewise, we humans have one body made up of many organs, with each serving its own God-given function.
The Placenta—an Unappreciated Organ
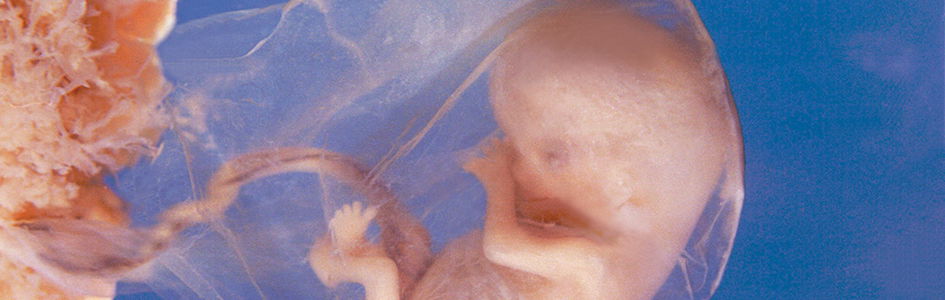
Of all the body’s organs, perhaps the one that best exemplifies selfless service is the placenta. Most people give little thought to the placenta, and few appreciate the marvelous complexity and profound importance of this organ that is discarded and forgotten after birth. While parents and loved ones lift joyful prayers of thanks for the safe arrival of their newborn, few think of thanking God for the essential services rendered by His marvelously designed creation—the placenta.
After the egg is fertilized, the placenta is the very first organ to develop. Recent studies show that when the fertilized egg divides to form the first two cells, one is already destined to form the placenta, while the other becomes the baby.
An Important Hormone-Producing Gland
As soon as three days after fertilization—weeks before the mother normally suspects she is pregnant—cells of the developing placenta, called trophoblasts, begin to produce hormones. These hormones ensure that the lining of the uterus—the endometrium—will be ready to receive the embryo’s implantation. Over the next few weeks, the developing placenta begins to make hormones that control the mother’s physiology in a way that ensures the proper supply of nutrients and oxygen, which are essential to the baby’s growth.
By about five days after fertilization the trophoblast cells, surrounding the developing embryo, begin to fuse together to form one giant cell with many nuclei (see Figure 1). This cell is called the syncytial trophoblast. One of the first functions of this placental giant cell is to invade the uterine wall of the mother in an amazing process called implantation (see Figure 2).
The placenta, sometimes called the “super organ” is evidence of the care and design of our Creator even at the earliest stages of life.
Prevents the Rejection of the Baby as a Foreign Graft
Although the developing placenta and baby implant within the thick nutrient-filled wall of the mother’s uterus, they are not actually part of the mother’s body. One of the placenta’s important roles is to protect the developing baby from an attack by the mother’s immune system, since the baby and the placenta are genetically unique and distinctly different from the mother.
It is still a mystery how the placenta prevents the mother from rejecting it and the baby as a foreign graft without shutting down her immune system.
After implantation, the placental giant cell “invades” the walls of several uterine arteries and veins, causing the mother’s blood to flow through channels within the cell (see Figure 3). When the baby develops its own blood and blood vessels, the mother’s blood and the blood of the developing baby come into close association, but they never mix or come into direct contact. The syncytial trophoblast forms a thin, seamless, and selective barrier between maternal blood and fetal blood. All the critically important nutrients, gases, hormones, electrolytes, and antibodies that pass from mother’s blood to the baby’s blood must travel across this seamless and selective filter. Waste products in the baby’s blood must, in turn, pass across this filter to the mother’s blood.
The Placenta Does It All!
In order to appreciate the marvelous work of the placenta, consider this: while the unborn baby’s vital organs are developing and maturing, they (with the exception of the heart) are essentially useless. The placenta serves the functions of these organs by working in association with the mother. With the help of the mother’s blood, the placenta must function as the baby’s lungs, kidneys, digestive system, liver, and immune system. The placenta does this so well that a baby can actually survive until birth even when one or more of these vital organs sadly fail to develop in its own body.
During the later part of pregnancy, the flow of maternal blood through the placenta reaches a rate of about one pint (.5 liter) per minute. To allow an adequate surface area for exchange between mother’s blood and baby’s blood, the interface between the two is folded and amplified in a complex way that resembles the trunks, branches, and twigs of trees (see Figure 4). There are typically about 20 of these tree-like structures (called cotyledons) in the mature placenta. The baby’s blood flows in vessels inside these cotyledons, whereas the mother’s blood flows all around the outside, like air blowing through a small grove of trees. The entire surface of all the tree-like cotyledons is covered by syncytial trophoblast, forming a seamless covering, which comprises a single cell with millions of nuclei (see Figure 5). This means that the entire surface of the placenta is covered by one giant cell, which has a surface area of over 100 square feet (9.3 square meters).
The Risky Expulsion of the Placenta after Birth
During the baby’s development, the placenta is securely attached to the endometrium of the uterus by some of the larger branches of each cotyledon. When the uterus contracts to expel the placenta after the birth of the baby, some of the endometrial surface is torn off with it. This results in severing about 20 large uterine arteries which, if unchecked, would involve the loss of blood at a rate of about one pint per minute. Since fewer than five quarts (4 liters) of blood are in the adult female body, all the blood would be lost in less than 10 minutes. It is also important to note that the blood-clotting mechanism is suppressed in the placenta and uterine blood vessels during pregnancy, creating a situation comparable to a hemophiliac with 20 severed arteries. These factors result in a wound that no one would expect to survive!
Saved by a Miracle!
How does a woman survive childbirth with such a wound? Here is another example of the awe-inspiring work of God, the Creator and Sustainer of life. You see, each of the severed uterine arteries has a precisely placed muscular sphincter that acts like a purse string, or a surgeon’s hemostat, to immediately close off the loss of blood. As a result, a normal birth involves the loss of only about a pint of blood. Simply amazing!
The next time you experience the joy of a baby’s birth, thank the Lord for providing this selfless placenta. And above all, reflect on the fact that our Creator, who at the time of childbirth so mercifully spares the mother from a fatal loss of blood, did not hesitate to shed His own blood in death to save us from sin, death, and the power of the devil.
Implantation of the Placenta
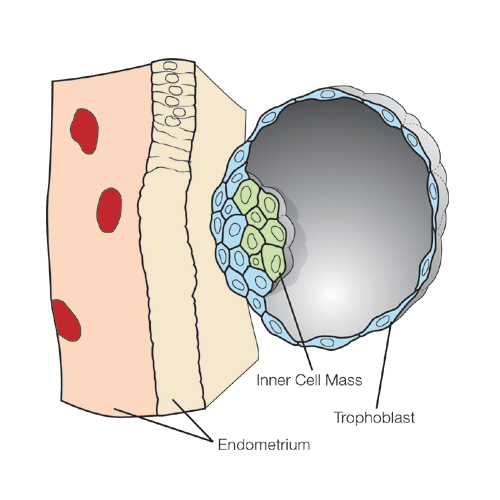
Figure 1
Cross-section through the blastocyst and uterine wall about five days after fertilization. The blastocyst is a hollow fluid-filled ball, and the amazing inner cell mass (shown in green) is the developing baby. The cells making up the wall of the ball are trophoblast cells that will form the placenta. The endometrium of the mother’s uterus (shown as a pink layer with red blood vessels and a tan layer of surface cells) is ready to receive the developing baby and its developing placenta.
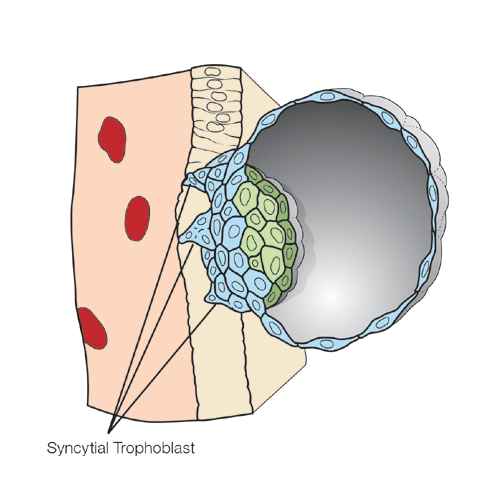
Figure 2
Cross-section through the blastocyst implanting into the uterine wall about six days after fertilization. At this time, trophoblast cells are progressively fusing together to form the syncytial trophoblast, which consists of a single giant cell with many nuclei.
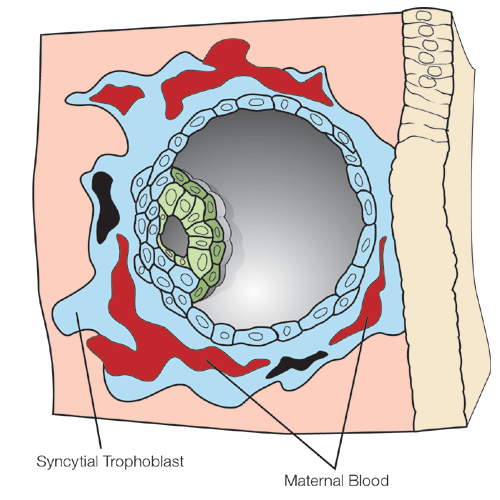
Figure 3
Cross-section of the blastocyst and endometrium about 12 days after fertilization. Maternal blood (red) is flowing into communicating spaces that develop within the giant syncytial trophoblast cell that covers the surface of the developing placenta (blue). The baby’s blood and blood vessels have not yet developed. The baby (embryo) has now developed into two layers.
Exchange of Nutrients
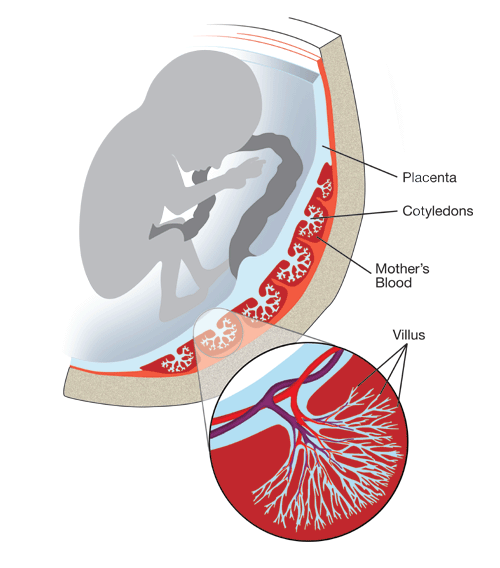
Figure 4
Cross-section through a third-trimester placenta with baby. The placenta (blue) consists of about 20 tree-like structures called cotyledons (see circular magnified area). The baby’s blood vessels, arriving by way of the umbilical cord, spread out within the placenta, sending a large branch into each cotyledon. Mother’s blood (darker red) intimately surrounds the cotyledons
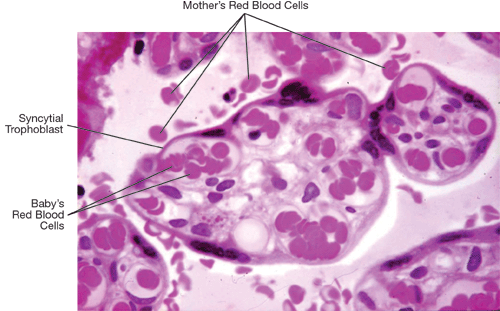
Figure 5
A microscope photograph of a cross-section of one of the smallest branches (called a villus) of a tree-like placental cotyledon at term. Mother’s red blood cells surround the villus, while the baby’s red blood cells are inside large capillaries within the villus. The blood of the mother and the blood of the baby are everywhere separated by the syncytial trophoblast, which is a seamless layer comprising a single cell.
Sources
- Larson, William J., Human Embryology, 2nd ed., pp. 33–47, 471–488.
- Moore, Keith L., The Developing Human: Clinically Oriented Embryology, 4th ed., pp. 104–130.
- Sadler, Langman’s Medical Embryology, 9th ed., pp. 31–49, 51–63, 65–86.
- Moore and Persaud, Before We Are Born, 5th ed., pp. 241–254.
- Junqueira, Carneiro, and Kelley, Basic Histology, 9th ed., pp. 421–445.
Visit The Bad News . . . and the Good News for a clear salvation message.
Answers Magazine
January – March 2007
This issue discusses topics such as gender equality, abortion, the origin of oil, racism, mand more.
Browse IssueRecommended Resources

Answers in Genesis is an apologetics ministry, dedicated to helping Christians defend their faith and proclaim the good news of Jesus Christ.
- Customer Service 800.778.3390
- Available Monday–Friday | 9 AM–5 PM ET
- © 2026 Answers in Genesis